You know that stiff, burning pain right above your heel? The one that makes your first steps out of bed feel like walking on broken glass? That’s your Achilles tendon screaming for help.
If that burning heel pain is localized strictly to the bottom of your foot rather than the back of your ankle, you are likely dealing with a different injury. Check out our guide to the best medical devices for plantar fasciitis to target bottom-of-the-foot pain.)
Here’s the problem: resting an Achilles tendon is nearly impossible if you want to walk, run, or even go to work. The tendon carries your full body weight with every step, which keeps tearing the inflamed tissue over and over again.
But here’s the good news: the right medical devices—from simple heel lifts to high-tech acoustic wave machines—can physically support the tendon, stop the micro-tearing, and speed up the healing process.
Let’s break down what actually works.
Best At-Home Recovery Gear & Braces
1. Compression Ankle Braces with Massage Pads
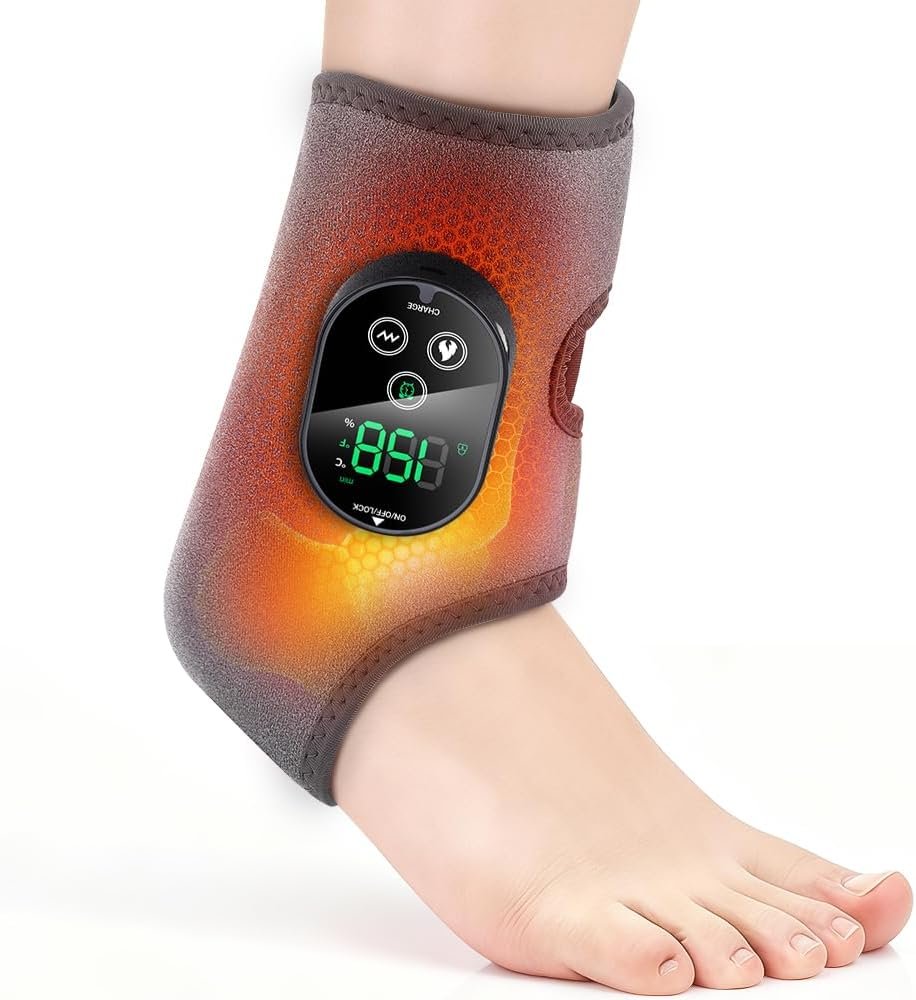
How it feels: A snug, warm squeeze around the ankle with gentle pressure on the sides of the tendon.
The benefit: Medical-grade compression improves blood flow to an area that normally gets very little circulation. Devices like the Aircast AirHeel and Bauerfeind AchilloTrain feature built-in silicone pads that physically massage the tendon as you walk, actively pushing swelling out of the area.
According to a 2023 systematic review published in the Sports Medicine & Arthroscopy Review, passive treatment modalities—including compression braces—led to greater short-term pain reduction compared to exercises alone. The study found that braces like the AirHeel provide immediate mechanical support while you rebuild strength through physical therapy.
Who should use it: Anyone dealing with mild to moderate Achilles pain who needs to stay active during recovery.
Who should avoid it: If you have poor circulation or diabetes-related neuropathy, check with your doctor before using any compression device.
2. Orthotic Heel Lifts and Cups

How it feels: A soft, supportive cushion that slightly elevates your heel inside your shoe.
The benefit: Standing flat on the floor stretches the Achilles. Inserting a simple silicone heel wedge shortens the tendon by raising your heel. This instantly takes the mechanical load off the injury so the fibers can rest without constant pulling.
Mayo Clinic recommends orthotic devices as a first-line treatment for Achilles tendinitis. They note that “a shoe insert or wedge that slightly raises your heel can relieve strain on the tendon.”
A 2021 randomized controlled trial compared heel lifts to eccentric exercises for midportion Achilles tendinopathy. Researchers found that heel lifts provided significant short-term pain relief, making them particularly useful in the early stages of treatment.
Who should use it: Anyone with insertional or midportion Achilles tendinitis who wants immediate relief while walking.
Who should avoid it: If you have severe biomechanical issues or other foot conditions, work with a podiatrist to ensure the lift won’t create new problems.
3. Adjustable Night Splints
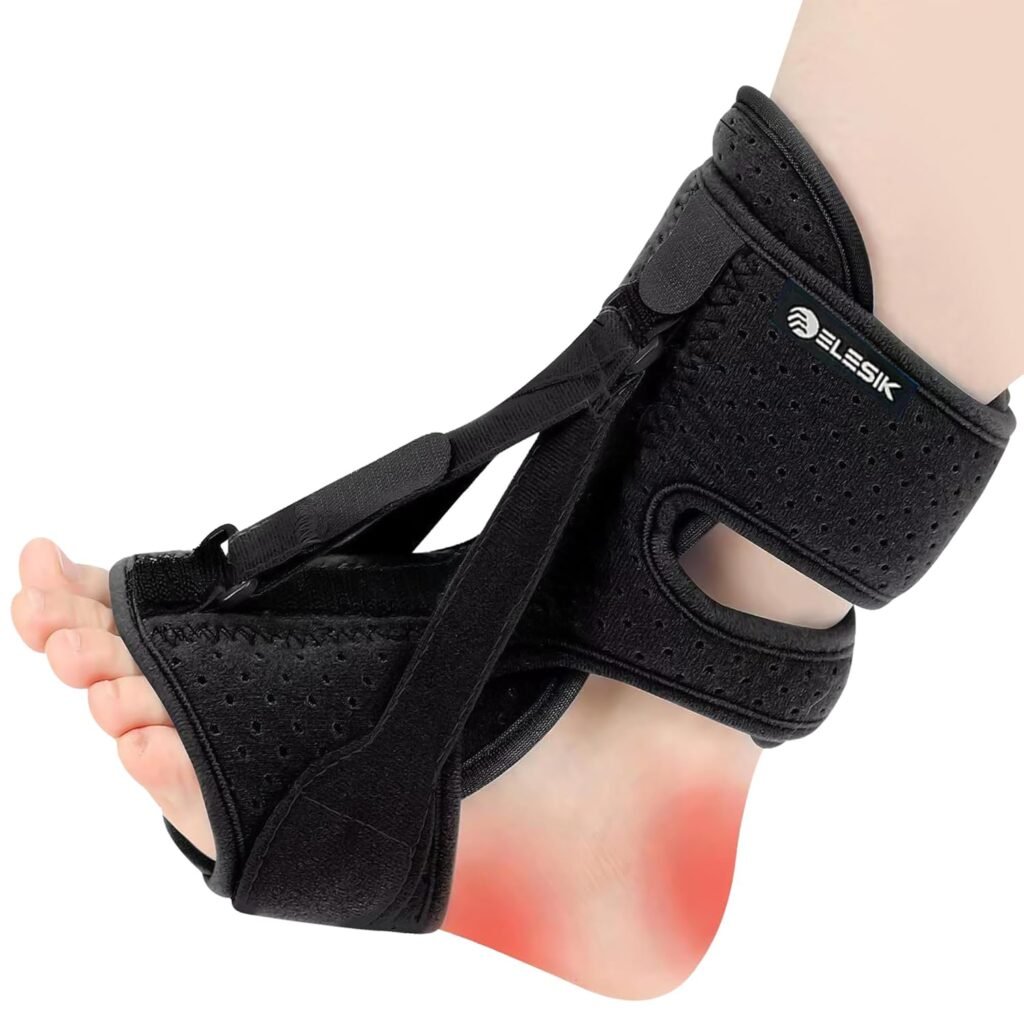
How it feels: A rigid but padded boot that holds your foot at a strict 90-degree angle while you sleep.
The benefit: Normally, your toes point down when you sleep, which causes the Achilles tendon to heal in a shortened position. When you stand up in the morning, the tendon rips again. A night splint stops this morning re-injury by holding the tendon in a stretched position all night.
However, the evidence is mixed. A 2008 randomized controlled trial published in the British Journal of Sports Medicine found that adding a night splint to eccentric exercises did not provide additional benefits for chronic midportion Achilles tendinopathy. Both groups improved significantly, but the night splint group showed no advantage in pain scores or patient satisfaction after 12 weeks.
That said, many patients report that night splints help reduce morning stiffness and pain. If you consistently wake up limping, a night splint might still be worth trying.
Who should use it: People who experience severe morning pain and stiffness.
Who should avoid it: Night splints can be uncomfortable and disrupt sleep. If you already have trouble sleeping, this might not be your best option.
4. Wearable Home Ultrasound Devices

How it feels: A warm, deep tingling sensation right over the sorest spot.
The benefit: Devices like the sam® wearable ultrasound are FDA-cleared for home use. They send continuous, low-intensity sound waves deep into the tissue. This increases local blood flow and speeds up cellular repair without requiring a trip to the physical therapist.
A 2021 systematic review in the Journal of Clinical Medicine examined low-intensity continuous ultrasound (LICUS) therapies. The research showed that LICUS significantly increased tendon breaking strength, tensile strength, and energy absorption in animal models of Achilles tendon injury. While more human studies are needed, early evidence suggests LICUS can support healing in Achilles tendinopathy.
The sam® device delivers therapeutic ultrasound for several hours per day, which differs from traditional 10-minute clinic sessions. This extended treatment time may enhance the biological effects on tendon repair.
Who should use it: Anyone dealing with chronic Achilles pain who wants a non-invasive, at-home treatment option.
Who should avoid it: Pregnant women and people with pacemakers should consult their doctor before using any ultrasound device. Do not use directly over open wounds or infections.
Advanced Clinical Treatments
1. Extracorporeal Pulse Activation Technology (EPAT)
What it is: A doctor uses a handheld device to send acoustic pressure waves straight into the damaged tendon. This treatment is also called extracorporeal shock wave therapy (ESWT).
How it works: These sound waves cause controlled microtraumas. This tricks your body into sending fresh blood, oxygen, and stem cells to the Achilles, forcing the tendon to restart the healing process.
Mayo Clinic describes ESWT as a noninvasive treatment that “sends shock waves to injured tissue to relieve pain and help with healing.” The procedure typically involves a series of sessions lasting 30 minutes or less. Side effects are usually mild and may include bruising, swelling, pain, numbness, or tingling in the treated area.
A 2023 meta-analysis of randomized controlled trials found that ESWT provided significant short-term pain reduction for Achilles tendinopathy, similar to other passive interventions. While the long-term effects need more study, ESWT is often used when self-care measures haven’t worked, but before deciding on surgery.
An ongoing clinical trial registered on ClinicalTrials.gov (last updated July 2025) is comparing ESWT to laser therapy for Achilles tendinopathy. The ESWT protocol involves 1,500-3,000 pulses at a frequency of 1-4 Hertz, delivered once a week for three weeks with one-week breaks between sessions.
Who should use it: People with chronic Achilles tendinitis who haven’t responded to conservative treatments like rest, physical therapy, and braces.
Who should avoid it: ESWT is not recommended for pregnant women, people with blood-clotting disorders, or those taking blood-thinning medications. Always discuss your medical history with your doctor before starting treatment.
2. Minimally Invasive Surgical Devices
What it is: If the tendon actually ruptures, doctors now use advanced tools like the TendMIN system.
How it works: Instead of cutting the whole back of the leg open, surgeons use this device to pass stitches through the tendon using a one-centimeter incision. This approach drastically cuts down recovery time and lowers the risk of infection.
The TendMIN system is FDA-listed and designed to enable percutaneous Achilles tendon repair through an incision of approximately 1 centimeter or less. As of February 2026, more than 100 U.S. clinical procedures have been performed using this system, reflecting sustained adoption across multiple hospitals and surgical centers.
Published research on minimally invasive and percutaneous Achilles tendon repair techniques has demonstrated potential benefits, including reduced infection risk, fewer wound complications, and accelerated recovery compared to traditional open repair approaches.
Who should use it: Anyone facing Achilles tendon rupture who wants to minimize surgical trauma and speed up recovery.
Who should avoid it: Minimally invasive surgery isn’t appropriate for everyone. Your surgeon will evaluate the severity and location of your rupture to determine the best approach.
Frequently Asked Questions
Does walking barefoot make Achilles tendinitis worse?
Yes. Walking barefoot forces your heel all the way to the ground, which fully stretches the Achilles tendon. This increased mechanical strain can aggravate an already inflamed tendon. You should always wear supportive shoes or use a heel lift when dealing with a flare-up.
Should I use a massage gun on my Achilles tendon?
No. You should never use a percussion massager directly on a tendon or bone. You can use it on your calf muscle to relieve tension, but using it directly on an inflamed Achilles can cause more damage. Tendons are dense connective tissue that don’t respond well to aggressive mechanical force.
How long does Achilles tendinitis take to heal?
With the right support gear and rest, mild cases can improve in a few weeks. Chronic cases can take several months. Mayo Clinic notes that catching it early and using proper braces, orthotics, and physical therapy can speed up the timeline significantly.
Take Control of Your Recovery
Achilles tendinitis doesn’t have to sideline you for months. The right combination of compression braces, heel lifts, night splints, and advanced therapies can give your tendon the support it needs to heal properly.
Start with simple, at-home devices like heel lifts and compression braces. If your pain persists beyond a few weeks, talk to your doctor about clinical treatments like ESWT or wearable ultrasound devices.